Improper Payment Rate
Skilled nursing facilities have one of Medicare's highest improper payment rates, roughly $5.9 billion annually.
Reduce errors and ensure accurate reimbursement with automated TripleCheck audits and Reimbursement Integrity Review.
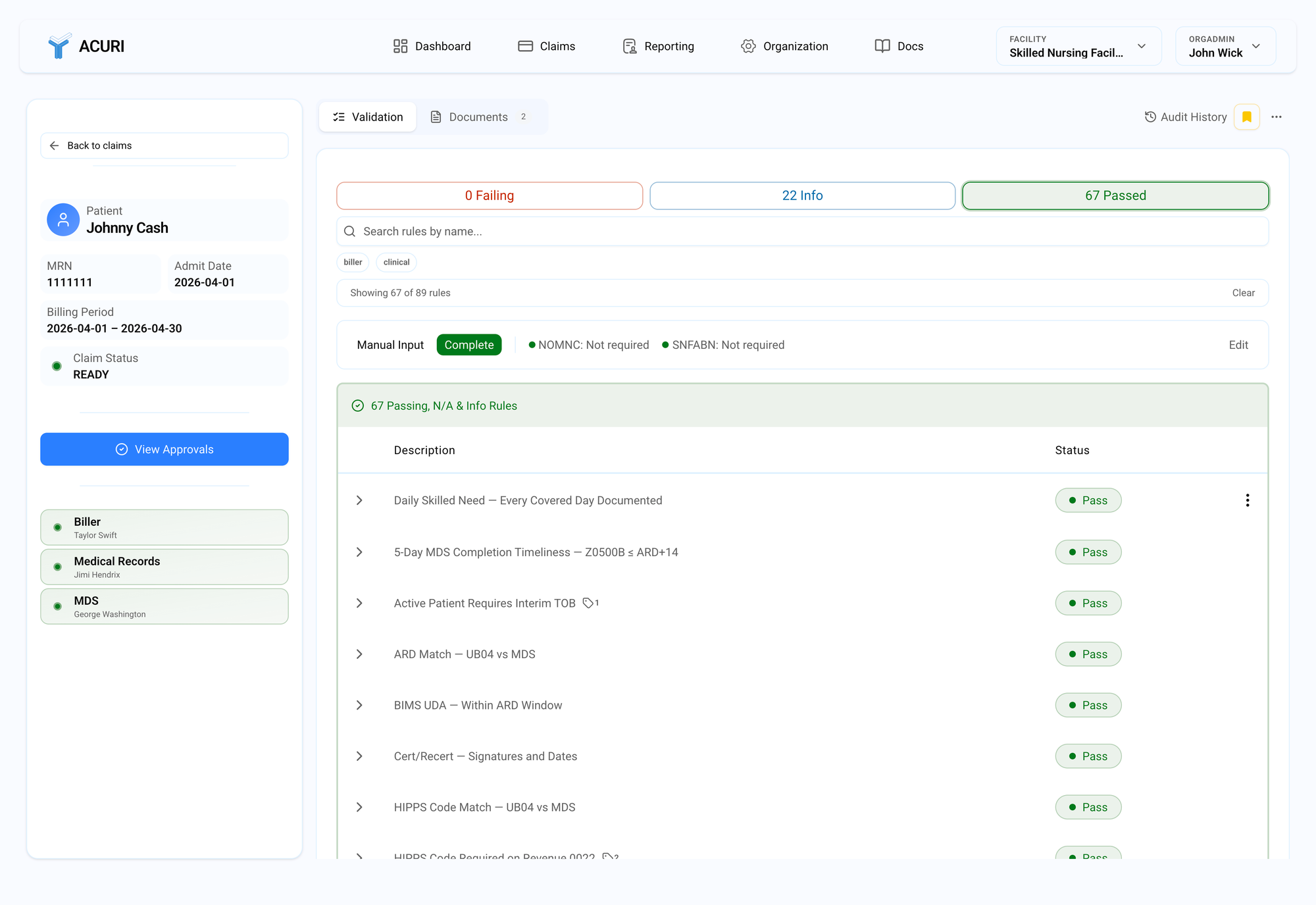
SNF billing compliance is complex, and mistakes are costly. Even small documentation gaps lead to millions in lost revenue and audit risk.
Skilled nursing facilities have one of Medicare's highest improper payment rates, roughly $5.9 billion annually.
Nearly 80% of these errors are due to insufficient documentation, meaning they're entirely preventable.
Medicare Part A SNF claims have an error rate around 15%, representing ~$4.8 billion in improper payments.
Acuri addresses these issues head-on, preventing errors before they happen and protecting your revenue with automated compliance checks.
See how quickly we pay for ourselves.
~700
claims / month
Volume is a Risk Multiplier: Your Medicare Part A scale turns small control gaps into enterprise-level exposure.
$10.5M
/ month
Estimated monthly dollars at risk: 700 Medicare A claims × $15,000 per stay.
$105K
/ month
Even when restricting the model to 1% of the CMS-reported error volume (14.9%), the financial impact totals $105K / month.
Finding just 1–2 issues covers your investment
At $15K per caught claim, recovering just $30K in prevented errors and Acuri pays for itself.
Based on 35 claims per facility per month at $15,000 average claim value. All figures shown monthly. Industry risk calculated using the CMS-published 14.9% SNF improper payment rate. Conservative estimate uses 1% — a fraction of the published rate.
AI powered automation that catches errors, validates billing accuracy, and gives your team confidence that every claim is compliant.
Our system performs comprehensive TripleCheck audits before submission: verifying documentation, checking coding accuracy, and ensuring compliance with Medicare Part A, Part B, Managed Care, and HMO rules.
Our AI validates MDS coding accuracy against clinical documentation, identifying discrepancies in diagnoses, NTA qualifiers, and therapy classifications to ensure every claim is defensible and accurate.
Get instant alerts for missing signatures, inconsistent coding, or documentation gaps. Track trends and improvements with comprehensive dashboards.
Join SNF providers who have recovered lost revenue and achieved compliance peace of mind.
Book Your Free Demo